Prior Authorization Metrics For Medical Items And Services (Excluding Drugs)
To comply with the CMS Interoperability and Prior Authorization final rule, Gold Kidney Health Plan is required to annually report aggregated prior authorization metrics on our website. Specifically, this includes a list of all medical items and services (excluding drugs) that require prior authorization, as well as data on prior authorization requests for those items and services (e.g., approvals, denials, etc.) over the previous calendar year. Publicly reporting these metrics promotes transparency and accountability, helps patients understand prior authorization processes, and enables providers to evaluate payer performance. In addition, metrics can be used to compare plans, programs, and payers. For questions on the data below, contact: Gold Kidney Member Services at (844) 294-6535 (TTY: 711).
Reporting Period: 2025
These are the medical items and services for which we require prior authorization (excluding drugs)
Click here for a list of all medical items and services that require prior authorization (excluding drugs)
Prior to January 1, 2026, impacted payers are required to send prior authorization decisions within the following timeframes:
- For MA plans and applicable integrated plans, 72 hours for expedited requests (urgent) and 14 calendar days for standard requests (non-urgent)
- For state CHIP FFS programs, 14 days for standard requests (non-urgent)
- For Medicaid managed care plans and CHIP managed care entities, 72 hours for expedited requests (urgent) and 14 calendar days for standard requests (non-urgent)
- For QHP issuers on the FFEs, 72 hours for expedited requests (urgent) and 15 days for standard requests (non-urgent)
There are no Medicaid FFS program required timeframes for either type of prior authorization request prior to January 1, 2026, and there are no CHIP FFS program required decision timeframes for expedited prior authorization requests prior to January 1, 2026.
Beginning January 1, 2026, the CMS Interoperability and Prior Authorization final rule requires Gold Kidney Health Plan to send prior authorization decisions within:
- 72hours for expedited requests (urgent)
- 7 calendar days for standard requests (non-urgent)
Standard (non-urgent) Prior Authorization Requests - Arizona
| How many times this happened | Out of total requests | Percentage | |
|---|---|---|---|
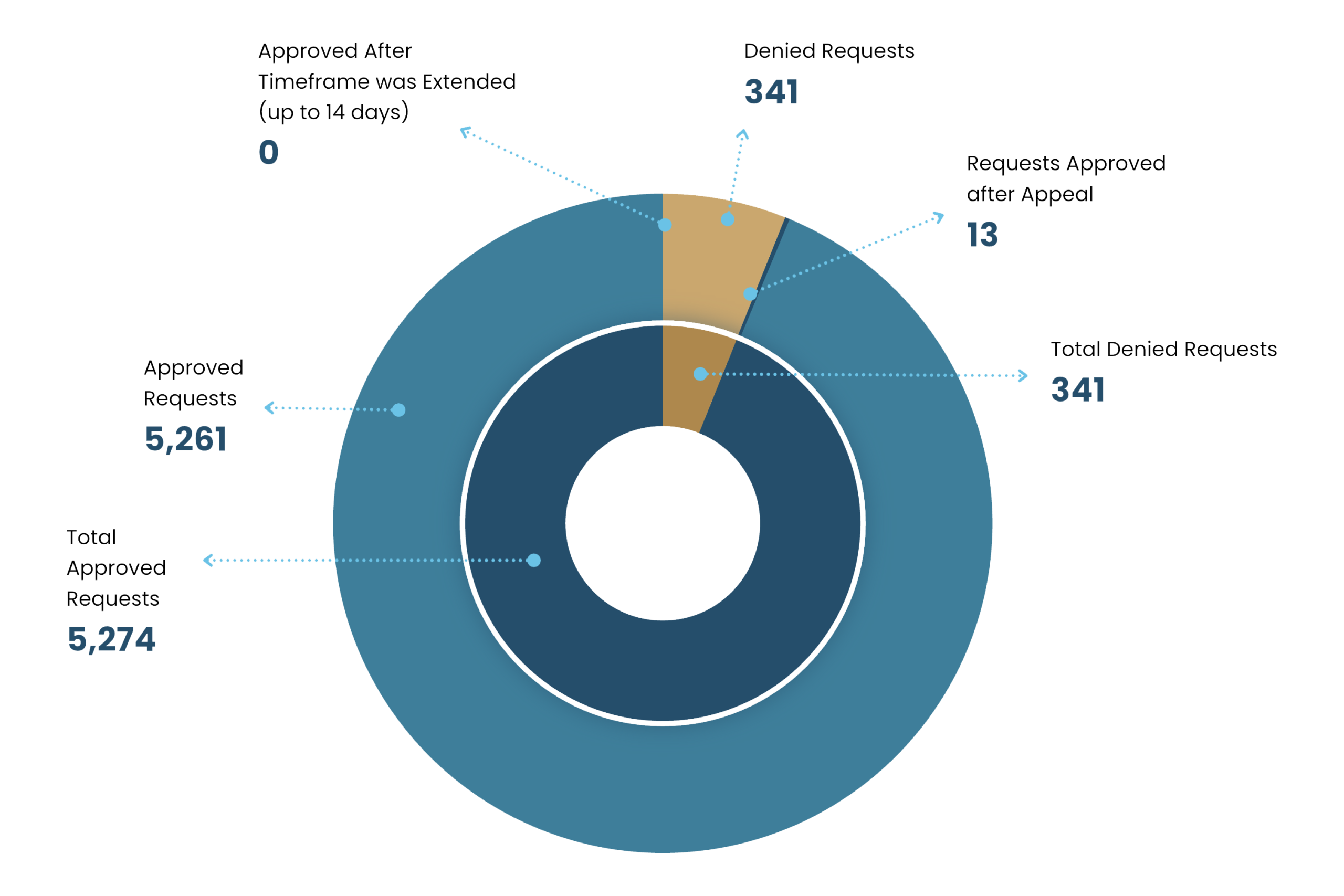
| Request Approved | 5274 | 5615 | 94% |
| Request Denied | 341 | 5615 | 6% |
| Request approved only after time for review was extended* | 0 | 5615 | 0% |
| Request approved only after appeal | 13 | 22 | 59% |
Expedited (urgent) Prior Authorization Requests - Arizona
| How many times this happened | Out of total requests | Percentage | |
|---|---|---|---|
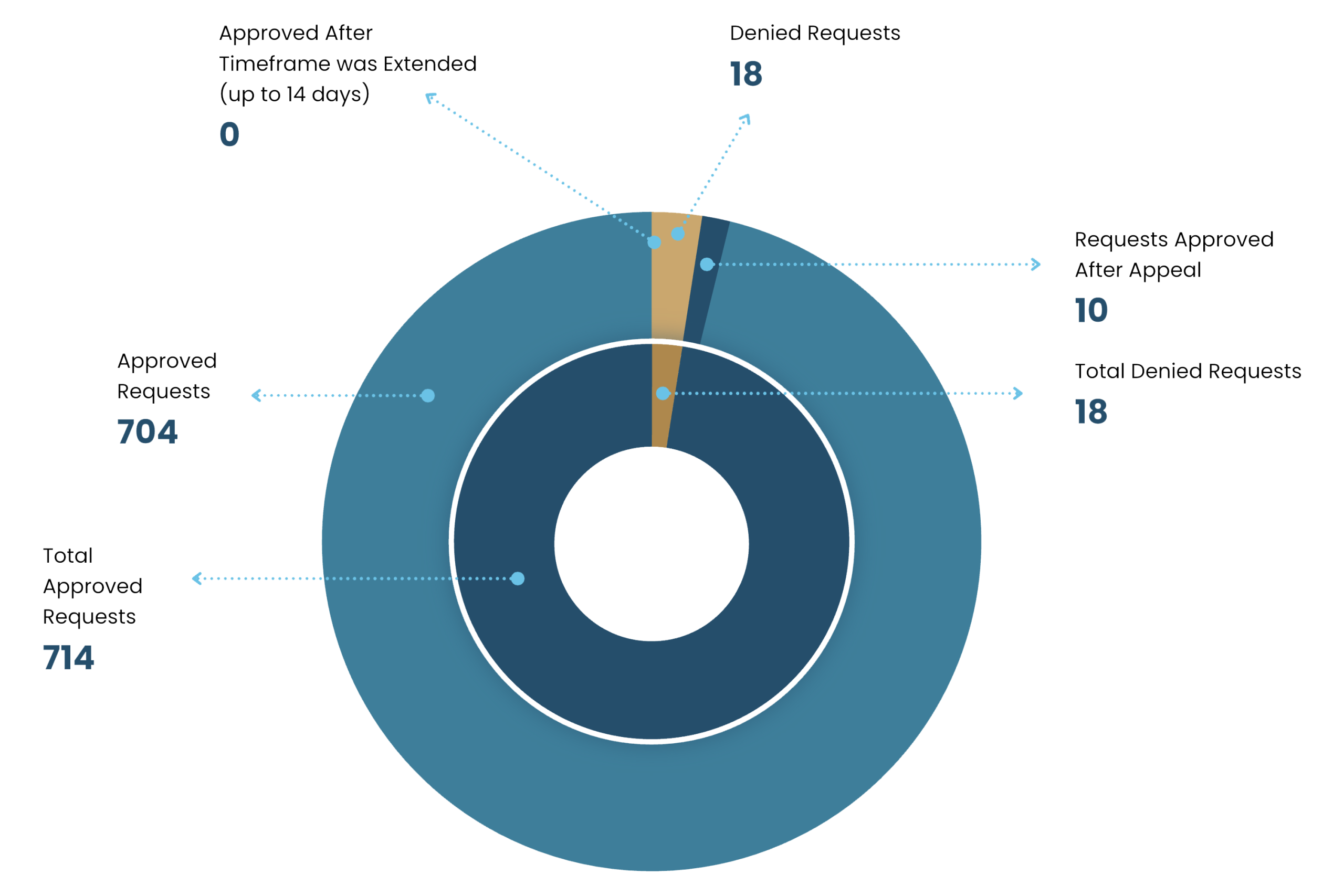
| Request Approved | 714 | 732 | 98% |
| Request Denied | 18 | 732 | 2% |
| Request approved only after time for review was extended* | 0 | 732 | 0% |
| Request approved only after appeal | 10 | 13 | 77% |
Time Between Receiving a Prior Authorization Request and Sending a Decision - Arizona
| Mean (Average) Time | Median (Middle) Time | |
|---|---|---|
| Standard (non-urgent) Prior Authorization Requests (response due to provider within 14 calendar days) | 3 Days | 2 Days |
| Expedited (urgent) Prior Authorization Requests (response due to provider within 72 hours) | 1 Day | 1 Day |
In 2025, we received a total of 5,615 standard (non-urgent) prior authorization requests for our covered patients in Arizona.
94% of those requests were approved:
3 Days
The median (middle) time that it took to make standard prior authorization decisions was
In 2025, we received a total of 732 expedited (urgent)
prior authorization requests for our covered patients in Arizona.
98% of those requests were approved
1 Day
The median (middle) time that it took to make standard prior authorization decisions was
1 Day
Standard (non-urgent) Prior Authorization Requests - Florida
| How many times this happened | Out of total requests | Percentage | |
|---|---|---|---|
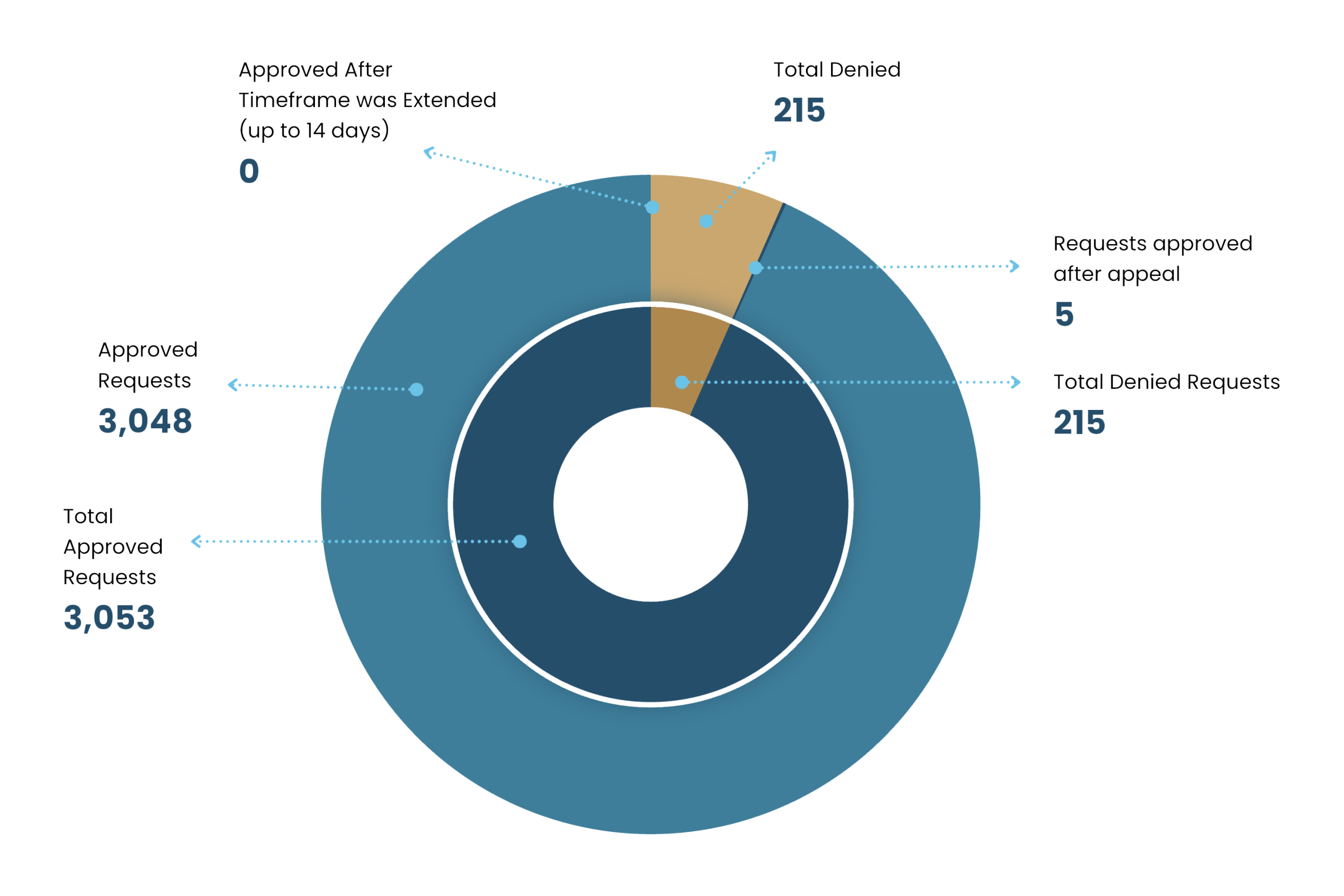
| Request Approved | 3053 | 3268 | 93% |
| Request Denied | 215 | 3268 | 7% |
| Request approved only after time for review was extended* | 0 | 3268 | 0% |
| Request approved only after appeal | 5 | 13 | 38% |
Expedited (urgent) Prior Authorization Requests - Florida
| How many times this happened | Out of total requests | Percentage | |
|---|---|---|---|
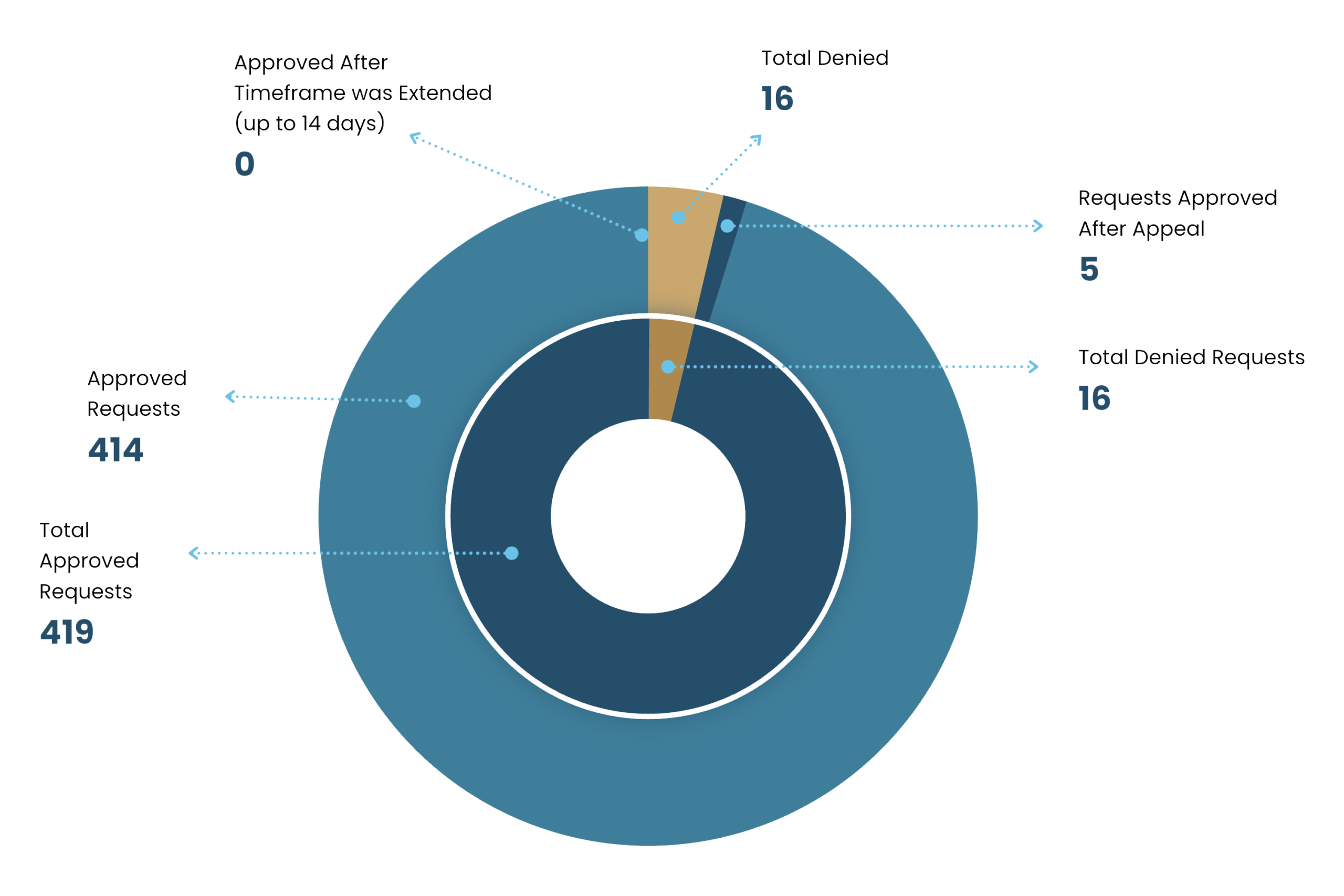
| Request Approved | 419 | 435 | 96% |
| Request Denied | 16 | 435 | 4% |
| Request approved only after time for review was extended* | 0 | 435 | 0% |
| Request approved only after appeal | 5 | 5 | 100% |
Time Between Receiving a Prior Authorization Request and Sending a Decision - Florida
| Mean (Average) Time | Median (Middle) Time | |
|---|---|---|
| Standard (non-urgent) Prior Authorization Requests (response due to provider within 14 calendar days) | 3 Days | 2 Days |
| Expedited (urgent) Prior Authorization Requests (response due to provider within 72 hours) | 1 Day | 1 Day |
In 2025, we received a total of 3,268 standard (non-urgent)
prior authorization requests for our covered patients in Florida.
93% of those requests were approved:
3 Days
The median (middle) time that it took to make standard prior authorization decisions was
2 Days
In 2025, we received a total of 435 expedited (urgent)
prior authorization requests for our covered patients in Florida.
96% of those requests were approved:
1 Day
The median (middle) time that it took to make standard prior authorization decisions was
1 Day
*It is optional to report the metric separately from the standard and expedited prior authorizations

